How chronic UTI forms
This picture commentary explaining the pathophysiology of chronic UTI is based on research at University College London (UCL) and is shared with permission from Professor James Malone-Lee. The late professor pioneered research and treatment for chronic UTI and was considered a leading global expert in the field. Each illustration is accompanied with detailed information describing the process. More information is available in the 2021 book Cystitis Unmasked.
These figures are drawn from experiments conducted on (1) mouse models of chronic cystitis and (2) more recent work done in our own laboratories [at University College London] using human bladder cells, or (3) our living culture of a human urothelium. The images are cartoons and the interpretation is a simplified analysis of a very complex situation

Figure 1
Figure 1 illustrates the bladder and urethra in health. The yellow part is the urine and at the bottom of the image there is a drawing of the urothelium (the tissue lining the bladder) which is about five cells deep. We believe that it takes about 100 days for a cell at the base to transit to the top surface. This is near a third of a year.

Figure 2
Figure 2 illustrates the circumstances during the early phase of a urinary infection. Note that the normal bladder is not sterile and contains at least 550 different species of bacteria so this is an idealised picture. We have shown bacteria called bacilli swimming in the urine. You will see that the urothelium is the same as before. It is probable that the normal bladder has plenty of microbes swimming around in the urine but they are in comfortable balance with the body and not causing symptoms.

Figure 3
In figure 3 there are changes in the urothelium. The bacilli have changed their form and have adopted the shape of round cocci. They have penetrated down to the base of the urothelium and in some cases they have entered the cells. This is called intracellular colonisation. In the mouse model we have found that if the infection is treated aggressively in the first 14 days then this intracellular colonisation will not occur. We suspect that this might be the case in the human and so we advocate very early and aggressive treatment of acute urinary infection until all symptoms have cleared. The microbes that have entered the cells will go into a dormant state similar to hibernation and so they will not divide. If microbes do not divide they will not be affected by antibiotics. This is a most important matter, the microbes inside the cells will not be affected by antibiotic attack until they start dividing, so by remaining dormant they survive short-lived antibiotic attacks. This is why assaults with powerful broad-spectrum agents or intravenous treatments are so disappointing. These methods produce early gratifying results by killing off large numbers of dividing microbes but once they are stopped the dormant microbes awake and invade the spaces cleared by the powerful agents. A single dormant microbe, woken from slumber, can become 1 million microbes before sundown.
Notice also that the GAG layer, a protein cap on the surface cells, has nothing to do with intracellular colonisation, so treatments designed to replace the GAG layer do not make much sense.

Figure 4
In figure 4 the situation seems to be getting more complicated. The cells that have become colonised have been transmitting distress signals to the immune system. This has resulted in an inflammatory response. If you look carefully you will see that the blood vessels have dilated up and this will cause the bladder wall to look red or inflamed. Some of these blood vessels might burst and leak blood into the urine which will be detected on dipstick analysis or microscopy. We have drawn some red blood cells floating in the urine with the bacilli. Just because the bladder looks red it does not imply a diagnosis of interstitial cystitis. If the inflamed bladder has a tendency to bleed spontaneously then it should be no surprise to see bleeding patches appear when the bladder is distended. It is claimed that this implies a diagnosis of interstitial cystitis – it does no such thing, it just illustrates the presence of inflammation.
The inflammatory response will also involve the infiltration of the urothelium with white blood cells (aka pus cells, leucocytes, neutrophils, polymorphs, inflammatory cells). These are attracted by chemicals called cytokines which are released by the parasitised cells. When the white cells arrive they fail to detect a problem because the microbes are hiding inside the cells. The white cells declare no problem and the urothelial cells disagree. This leads to a standoff and results in a chronic inflammatory response that does not achieve very much other than cause pain and white blood cells in the urine. This situation is responsible for the chronic low-grade symptoms that patients describe and which may persist despite apparently normal urinalysis. If the reaction is low-grade white cells are less like to leak into the urine. A culture is unlikely to find the problem because the pathological microbes are imprisoned inside the urothelial cells and are not in the urine, which is collected for culture.

Figure 5
Figure 5 illustrates a further stage in the evolution of the persisting inflammation. The urothelium thickens. All epithelial tissue will thicken, through a process called metaplasia, when stressed in any way. The skin of the feet shows this through the formation of corns caused by poorly fitting shoes. The purpose of the thickening is an attempt to form a protective barrier; but it is not very effective since the offending microbes are inside the cells. Given this occurrence, it will take longer for a cell at the base to reach the surface.
This thickening of the cellular part of the urothelium contradicts the unproven ideas about GAG layers and drugs that encourage replacement of the GAG layer. There is no evidence for GAG layer deficiency, instead the urothelium is laying down a barrier made of many cells and vastly thicker than a GAG layers or any other surface protein. It is no surprise that a 2016 analysis of 36 randomised controlled trials, evaluating 1,822 participants conducted on the use of bladder instillations showed that they are no better than placebo. There is no coherent pathophysiological reason for why they should work.
Some years ago there was a flurry of interest in bladder wall thickness detected by ultrasound in patients with lower urinary tract symptoms. Eventually this observation was found not to correlate with urodynamic study data from cystometrograms and interest waned. This was a pity because the bladder wall thickness may carry a more relevant message than people assume. However, it supports the experience, demonstrated in clinical trials, that urodynamic studies shed no light on this condition and should have no role to play.
The inflammation and the increased number of urothelial cells will also thicken the wall of the urethra. This causes a degree of obstruction and thus we find that the most sensitive symptoms of infection are the voiding symptoms: Hesitancy, reduced stream, intermittency, terminal dribbling, post-micturition dribbling and double voiding. Some surgeons recommend urethral dilation as a treatment, but that is to confuse cause and effect: The voiding problem is not causing the infection it is the other way round. A similar muddle influences concerns about incomplete bladder emptying; the inflammation leads to a degree of urinary retention that can be resolved by treating the infection and not by using intermittent catheterisation. There is no good reason why a volume of urine left behind in the bladder after voiding should cause infection. Some patients with severe attacks of infection can develop acute urinary retention.
The thickened and inflamed bladder wall will reduce the bladder capacity and the inflammatory chemicals may cause the bladder muscle to contract inappropriately leading to frequency, urgency and urge incontinence. Pain may also play a role in a low bladder capacity. Stretching the bladder by hydro distension or cystodistension is not going to help this situation at all but it will surely make the bladder wall bleed. This figure shows red blood cells in the urine which can be a manifestation of chronic inflammation anyway.
The published literature shows no evidence of benefit from cystodistension or urethral dilation. That is not so surprising since stretching was never thought to help with an inflammatory infiltration causing metaplasia.
The metaplasia of the bladder can be seen on cystoscopy where plaques and fronds on the bladder wall, notably at the trigone, are evident. Some surgeons cauterise such lesions. Why should that help? If you want to burn away the chronic infection, you would really have to set fire to the whole bladder. How will cauterised bladder urothelium repair in tissue that is harbouring a chronic infection?

Figure 6
Figure 6 introduces another phenomenon, which is the formation of biofilms. The human body is covered in biofilms. Wherever there is a surface, biofilms will form. Our skin, eyes, intestines and bladder are covered in biofilms and we are discovering more inside the body. Biofilm formation is not a disease process. However, if a pathological microbe gets into a biofilm two properties come into play: (1) the microbes cease to divide and therefore become unsusceptible to antibiotic attack. (2) they become attached to the cells either inside or outside. Thus these biofilms can harbour dormant pathogens with the ability to break out, divide and set up fresh infection.
It is best to think of the intracellular microbes and the biofilms as one pathological state involving the parasitisation of the cells.
It is nonsense to think that by drinking a great deal you will wash away the infection. These microbes are glued to the cells and cannot be washed away. High fluid intake results in dilution of the urine and of the antibiotic and the natural anti-infection chemicals produced by the urinary tract. If a urinalysis test is positive, and you are told to drink plenty of fluids, the test may become negative due to the dilution effect and not disease cure.
In this image we show white blood cells or pus cells in the urine. Counting these cells is our most important pathological outcome measure. The white cell count (pyuria) is the best marker of urinary infection known, provided that it is conducted on an immediately fresh, unspun, unstained specimen of urine examined using a microscope and a haemocytometer counting chamber.

Figure 7
Figure 7 shows the crux of the matter. The body’s innate immune system responds to the cellular infection by shedding the cells and this is a most effective way of clearing the problem. However, the microbes have evolved to detect the fact that they are inside a free floating cell that is dying and on its way to the sewer. The bug must escape and does so by waking up, dividing vigorously to create a microbial swarm that then bursts out of the cell into the urine. Continued division causes many more microbes to form what we call a “planktonic flare” which can lead to an acute cystitis, but it will also result in colonisation of healthy fresh cells at the base of urothelium. Thus, the parasitisation process is reproduced. When we treat, we depend heavily on the innate immune shedding of cells and support this process by using antibiotics and antiseptics to attack any microbes that escape from the cells. From time to time, a microbial swarm may overwhelm this support and an acute flare develops despite treatment being in place. In those circumstances we rescue the situation by increasing the dose of the regimen on the principle that higher concentrations will overcome the increased microbial load. We have to maintain the treatment regimen until all the parasitised cells have been cleared and that takes time.

Figure 8
Figure 8 We focus on the persister microbes dormant in the cells of the bladder wall. For clarity we have left out several the other features of a chronic infection. Over to the left we start with a single microbe, dormant inside a cell. We call this a persister. For some reason this microbe may wake up and start dividing and this is shown in stages as you move to the right. As the cell fills with dividing microbes it becomes damaged and dividing microbes leak out into the tissue spaces. This will cause an acute flare. Eventually the cell perishes, and the microbes continue to divide through the tissue spaces and if they are given the chance they will set up new, dormant, persisters inside fresh cells. Whilst the microbes are dividing they will be particularly susceptible to antibiotic attack and therefore we increase doses during an acute flare. We seek to achieve the highest concentrations of antibiotic in the tissues that we can. This diagram explains why short-lived courses of powerful antibiotic can induce a gratifying immediate response only for the symptoms to return in a few weeks. The short antibiotic course does nothing to the root of the problem which is the existence of dormant persister microbes that are really behaving like seeds waiting for the right moment to break out again.
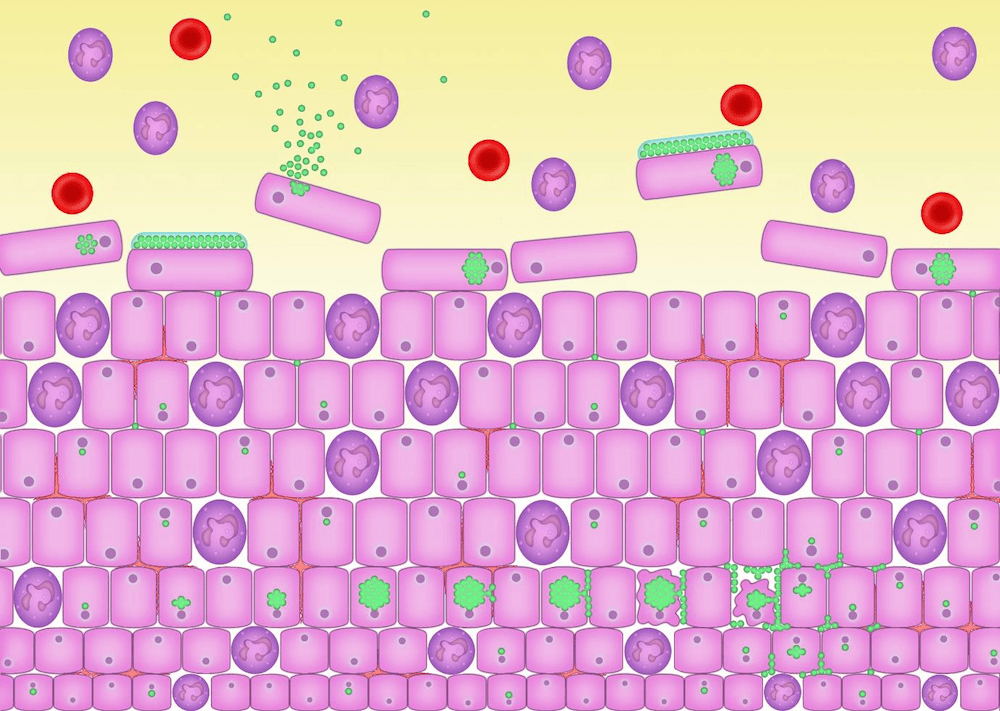
Figure 9
Figure 9 In figure 9 we put it all together. It is worth spending time studying this and absorbing the information that is there. Always remember that these images are cartoons. If we showed you the photomicrographs from our laboratory series, it would be very difficult to appreciate the patterns. We must use special stains and different light filters to make sense of the complexity.
Click on the image below to download the Chronic Urinary Tract Infection Picture Commentary PDF by Professor James Malone-Lee
Attributions
The Chronic Urinary Tract Infection Picture Commentary is shared with permission given by the late Professor James Malone-Lee MD FRCP in 2018, then Emeritus Professor of Medicine at University College London (UCL), United Kingdom. Professor Malone-Lee established an NHS outpatient clinic, the Lower Urinary Tract Service (LUTS) at the Whittington Hospital and a private chronic UTI clinic that is now managed by his son, Dr Matthew Malone-Lee. Dr Malone-Lee’s team of doctors continue to offer assessment, diagnosis and treatment for chronic UTI. The management program is based on the research findings from Professor Malone-Lee’s former academic program at UCL. You can contact Dr Malone-Lee’s Artemis Cystitis Clinic (10 Harley Street, London) by email for more information: clinicadministration@artemiscystitis.com You can also watch our 2021 interview with Professor Malone-Lee on our Youtube channel.
